| By K. Lee Lerner |
Most people are trying to put the COVID-19 pandemic, with all its tragedies, disruptions, uncertainties, and inanities, in the rearview mirror. The World Health Organization (WHO) declared the COVID-19 global health emergency on May 5, and the United States declared the public health emergency on May 11. Budget realities mean that governments and public health agencies are scaling down testing. WHO recently estimated a 90 percent reduction in global COVID–19–related variant testing and reporting compared to levels in November 2021 during the Omicron variant outbreak.
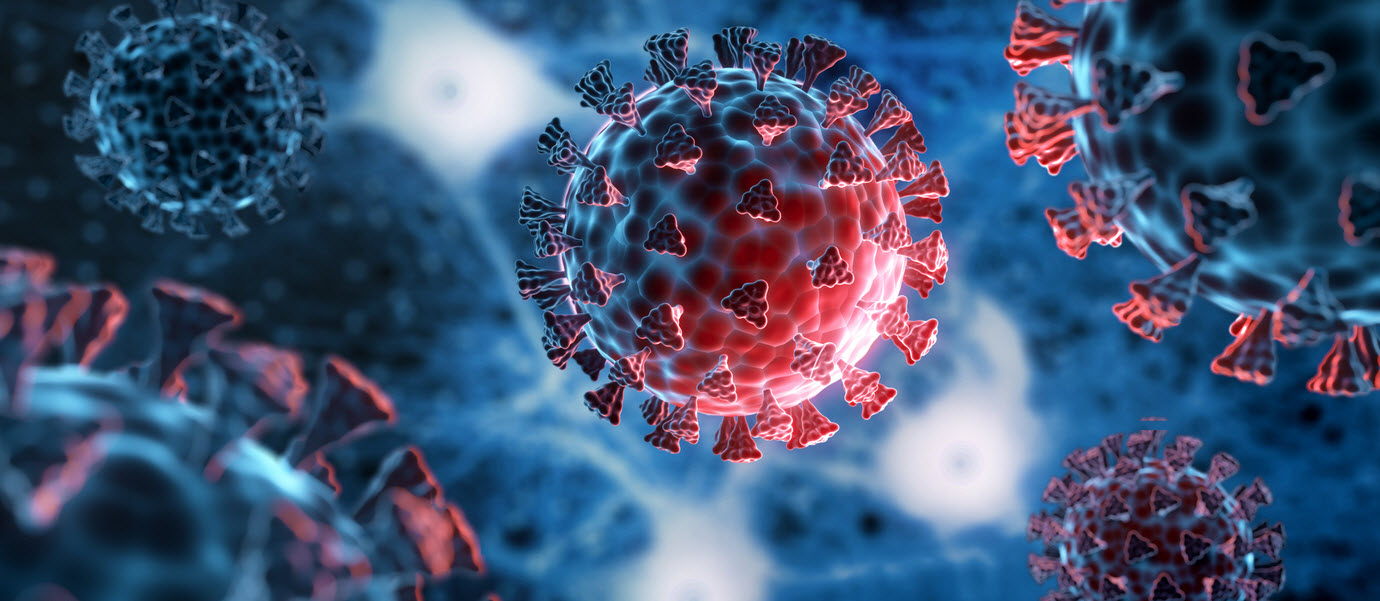
Yet the SARS-CoV-2 virus responsible for COVID-19 keeps evolving. Natural evolutionary mechanisms ensure that genetic mutations and changes create new COVID-19 variants. Not that every new variant is potentially more transmissible or lethal (in fact, most are not), but the combination of greatly reduced testing and sequencing combined with the evolution of highly mutated variants like the BA.2.86 variant, discovered in July 2023, indicates a need to potentially shift vaccine strategies that have been primarily oriented to protecting against specific widely circulating variants.

In essence, biotechnology firms and vaccine manufacturers can easily be placed in a position where they are chasing variants with vaccines. In the time needed to develop, test, gain approvals, produce, and distribute new vaccines, boosters, and medicines, new variants arise. The most prevalent variant challenging immune systems around the world may no longer be the variant targeted by the vaccine, booster, or medicine.
This doesn’t mean new vaccines and boosters won’t offer some protection (especially against severe illness or death), but given the placement of mutations that give rise to the new variants, they could stimulate the production of antibodies less effective or ineffective against a prevalent circulating variant.
The new monovalent booster expected to have been ready last month is, for example, designed to protect against what has recently been the most widely circulating XBB.1.5 variant. It is possible, however, that by the time the shots are given, BA.2.86 may be challenging—or have replaced XBB.1.5—as the most prevalent variant causing illness in parts of the world.
The appearance of hypermutated variants also doesn’t mean that the world’s population faces the same risks it faced with the spread of the novel SARS-CoV-2 virus, responsible for the first outbreak of COVID-19 in Wuhan, China, in late 2019 or early 2020. Even if a new variant was completely immune evasive (i.e., antibodies produced by prior exposure, illness, vaccines, or boosters become less effective), the antibody response is only the first tier of the human immune response. The next line of defense, T-cell–mediated immune response, still normally offers people some broad immunity.
A shift to variant-proof vaccines using broad neutralizing antibodies is already the focus of several research efforts, with candidate vaccines developed by teams at CalTech and Walter Reed currently in phase 1 trials.
The new BA.2.86 variant is a hypermutated variant that has radically departed from the normal progression of variants. The 36 new mutations on BA.2.86’s spike protein more than double the prior total accumulation of 30 mutations on the Omicron variant spike protein that had evolved from the original SARS-CoV-2 virus, responsible for the first outbreaks of COVID-19.
Mutations on the spike protein are critical because the spike protein is involved in receptor recognition, viral attachment, and viral entry into host cells.
The mutations on the BA.2.86 spike protein also double the number of mutations found on the spike proteins of currently widely circulating variants (e.g., XBB.1.5, EG.5.1, and FL.1.5.1). Moreover, 16 of those mutations are known to facilitate immunological escape.
No one is yet predicting another wave of severe illness from BA.2.86, and the cases that have arisen in Denmark are, thus far, unremarkable. Currently, there is also no evidence that the virus spreads as fast as the Omicron firestorm, but confidence in that assessment is hindered by a lack of testing. Should WHO classify BA.2.86 as a variant of concern like Omicron, it would be designated as the Pi variant.
As of August 24, 2023, at least nine cases have been attributed to BA.2.86 in five countries (Denmark, Israel, Switzerland, the UK, and the United States). BA.2.86 has also been found in wastewater samples and at airport screenings in countries without reported cases. While cases in Denmark, where BA.2.86 was first detected in July, haven’t spiked, it may be spreading quickly because the genomes of specimens taken from the cases reported appear remarkably consistent, meaning the virus has little time to incorporate additional mutations.
Thankfully, public health agencies and clinics can easily detect BA.2.86’s unique signal on a standard PCR test, and that means that the variant is easier to track.
While there is no evidence that BA.2.86 causes a more severe form of COVID-19 than the Omicron variant, the number and placement of mutations mean that makers of antigen tests, Paxlovid, and vaccines will be on alert and testing to see how these measures handle the variant. While tests have shown that the anticipated XBB.1.5 booster is also effective against the EG.5.1 and the FL.1.5.1 variants, the number and location of mutations in BA.2.86 induce uncertainty in how effective the new booster might be against the BA.2.86 variant.
 About the Author
About the Author
K. Lee Lerner is a writer, editor, and aviator who, along with Brenda Wilmoth Lerner, is the editor of the Gale Encyclopedia of Espionage, Intelligence, and Security; Climate Change: In Context; and many other award-winning books and articles on science, technology, and a range of global issues. A full bio and list of his work may be found at https://scholar.harvard.edu/kleelerner and https://harvard.academia.edu/KLeeLerner/.