| By Brenda Wilmoth Lerner, RN |
For some time, just prior to the COVID-19 pandemic taking center stage, which dominated both the research and clinical scenes for more than three years, scientists were beginning to make progress on another widespread health threat that can affect people of all ages—sepsis. Now, as we enter the 2023 respiratory illness season, with influenza, respiratory syncytial virus (RSV), and COVID-19 all expected to circulate in our communities, it’s time to talk about sepsis again.
Sepsis is a potentially life-threatening systemic response by the body to an infection. It usually follows a bacterial infection but can also develop as a result of a viral, fungal, or even a protozoan infection. In fact, research from Harvard University recently found that infection with the SARS-CoV-2 virus resulted in sepsis more often than was initially assumed during the pandemic. Influenza complications such as pneumonia are also notorious preceptors of sepsis, especially in the elderly and other vulnerable populations. This is why sepsis awareness is important during the flu season—because early recognition and treatment of infections are vital to saving people’s lives.
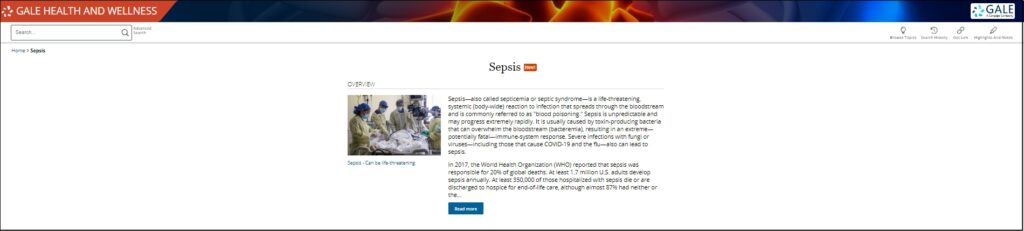
Each year in the United States, about 1.7 million people develop sepsis, and at least 270,000 people die from it. Although anyone with an existing infection can develop sepsis, some people have an elevated risk for the condition: infants less than 12 months of age; adults 65 and over; people with chronic health conditions including diabetes, kidney disease, lung disease, or cancer; people with a compromised immune system; people with a recent severe illness, a recent hospitalization, or a recent wound or trauma; and people who have previously survived sepsis.
Most infections that lead to sepsis develop outside of the hospital, and many people who develop sepsis initially sought treatment for common respiratory, skin, or gastrointestinal infections. During the cascade of events that occurs when sepsis develops, immune and inflammatory responses go into overdrive, quickly stressing organ function, metabolism, and fluid balance. Symptoms can include either a high fever or a temperature below 38 degrees Celsius (100.4 degrees Fahrenheit), vomiting, pain, difficulty breathing, fatigue, an elevated heart rate, confusion, and chills. The skin may appear mottled, discolored, or streaked due to impaired circulation. Babies may become lethargic and have reduced urine output.
Because most of these symptoms overlap with flu or other common infections, doctors advise people experiencing the flu, gastroenteritis, COVID-19, skin infections, or other common infections to be on the lookout for worsening symptoms and to seek treatment quickly when they occur. Sepsis can proceed to septic shock, which includes organ failure and faltering blood pressure, within hours. About 80 percent of people who develop septic shock will die from sepsis.
Just before the pandemic began in late 2019, data from the results of a study published in the Journal of the American Medical Association showed that six years of efforts toward reducing deaths from sepsis was beginning to work in New York state hospitals. The key to this improvement was a set of protocols known as Rory’s Regulations, named after Rory Staunton, who died in 2012 at age 12 of sepsis resulting from an infected scrape on his leg. Rory’s parents successfully advocated through their End Sepsis foundation for the protocols, which were mandated for New York hospitals in 2016; they outline screening measures to rapidly identify sepsis cases and to initiate treatment within hours.
The Centers for Disease Control and Prevention (CDC) soon followed with the national Hospital Sepsis Core Elements (HSCE) and the Get Ahead of Sepsis campaigns. The HSCE provide guidance for implementing standardized processes to screen for sepsis and to initiate rapid treatment. The Get Ahead of Sepsis campaign focuses on sepsis awareness and education for both the public and medical workers. In your doctor’s office, or if you find yourself in an emergency room this flu season, you might see a CDC campaign poster asking, “Could this be sepsis?” or advising you to take action to “Get Ahead of Sepsis.” Recommended actions include preventing infections with vaccines and by receiving regular care for chronic health conditions, practicing good hygiene by washing hands frequently and keeping cuts clean and covered until they heal, knowing the signs and symptoms of sepsis, and by acting fast to seek treatment if an infection doesn’t improve or worsens.
Information on just about any bug that could affect you and your family this respiratory illness season is available in the Gale Health and Wellness database—COVID-19, RSV, influenza, strep throat, and common colds included. Fortunately, for most people, these illnesses resolve with treatment, rest, and time, or are prevented altogether with vaccines. But for safety’s sake, please consider taking a look at the new sepsis portal in Gale Health and Wellness.